Why Varicose Veins Develop & When to Treat (Not Wait)
Updated December 2025 from original 2016 article by Dr. Janna Bentley
Women often ask, “Why me?” when it comes to their spider and/or varicose veins. These annoying entities are not only unappealing to look at, but can cause significant pain and seriously impact your quality of life. In fact, they are common (estimates are as high as 60% in the general adult population in North America), and become even more so as we age.
The answer comes down to two things:
- How veins physically function
- Which risk factors are present
What’s Actually Happening Inside Your Veins
Physically, veins function to return blood to the heart. The veins in our legs have a big job to do as they are often working against gravity to move blood uphill when we are standing. Our calf muscles act as pumps. As you walk, your muscles squeeze the veins, milking the blood inside them upwards. You may have heard of soldiers standing at attention for hours at a time and passing out. To prevent this they are told to pump their calf muscles every once in a while to keep blood from pooling in their legs. As a result of the pumping action they keep blood flowing from their legs, back up to their hearts and ultimately to their heads, decreasing their chances of fainting.
There are one-way valves every few centimetres inside our veins that should keep the blood flow moving towards our hearts. This means that when your leg muscles are relaxed, i.e. when you’re standing still, there should be no backflow of blood. This is where things can go wrong and you start to develop spider and varicose veins. Spider veins are just smaller versions of varicose veins, albeit with some minor differences.
Valves are made up of leaflets that should meet and completely seal off the vein when they are closed. The valves are forced open with muscle contraction and close when our muscles relax. If the leaflets don’t quite meet, there is a constant trickle backwards of blood inside the vein. Any point in the vein below the leaky valve is now vulnerable and begins to change as it has to deal with more blood from the backflow.
In response to the backflow and added volume of blood, our veins dilate, twist and turn, and become thicker and more obvious to the naked eye. We start to notice them as they are unattractive and can begin to cause discomfort, especially in hot weather and after being on our feet all day. Besides their unappealing look, spider and varicose veins can cause significant throbbing, aching, heavy, and tired feelings in our legs. There are other associations as well including: restless legs, night cramps, itching, swelling, darkening of the surrounding skin, ulcer formation, and inflammation of the veins themselves (thrombophlebitis).
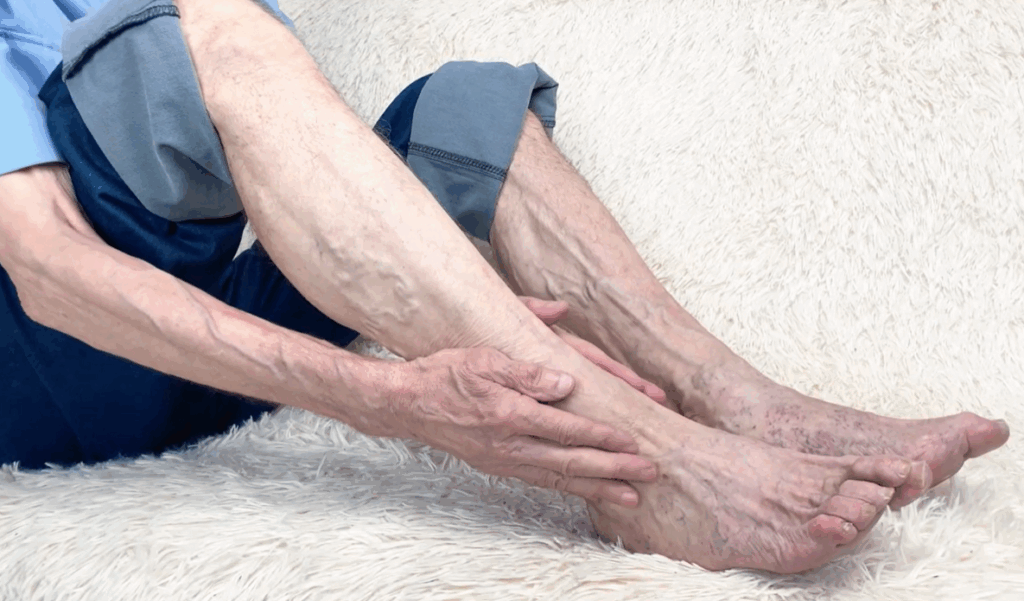
In 2025, believe it or not, the fundamentals of the human body have not changed. The underlying mechanisms remain the same, but we can diagnose these issues using ultrasound-guided vein assessments, which allow us to map exactly where valves are leaking and how severe the reflux is.
Why Varicose Veins Develop: Key Risk Factors
Besides the physical makeup of veins, there are risk factors that you may have leading to spider and varicose vein formation. Some of these you can change and others you can’t.
1. Female hormones & pregnancy
The #1 risk factor is being female – at least 95% or more of the patients we see in our clinic are female. This is largely due to the female hormones estrogen and progesterone. Women are the ones who carry pregnancies and this pregnancy state wreaks havoc on veins. The increased pressure of the growing womb puts strain on our leg veins in addition to higher levels of hormones circulating in our bodies at that time. Birth control pills and hormone replacement therapy can cause worsening of spider and varicose veins. These hormonal influences remain one of the biggest contributors we see in 2025.
2. Heredity (Family history)
The next biggest factor leading to spider and varicose veins is heredity. If you have spider and/or varicose veins you probably can think of at least one relative who does as well. It is often inherited from mothers or grandmothers. It is thought that the tendency towards leaky valves is what begins the whole pattern, and this is what tends to be passed down.
3. Age (especially 40s–50s)
Often the women we see who have noticed a sudden increase in the number of spider and varicose veins on their legs are in their forties or fifties. Studies have shown that it’s around menopause or in the period just before that our veins become significantly weaker. They become less able to adapt and become varicosed more easily.
4. Height and weight
Height and weight also play a role in spider and varicose vein development. The taller you are the heavier you are, meaning more strain placed on your veins. Luckily your weight is one of the risk factors over which you have some control.
5. Physical fitness
Physical fitness not only decreases your weight, but at the same time leads to a more efficient calf-muscle pump. This helps your veins to better perform their job of returning blood to the heart, with larger muscle bulk giving more support to the veins they pump.
6. Sedentary lifestyle
It’s interesting to notice that westernized populations are much more likely to have spider and varicose veins. This is likely linked to our more sedentary lifestyles and physical fitness levels in North America. In 2025, prolonged sitting especially with modern desk work and remote work culture, continues to contribute significantly.
7. Injury or trauma
The last risk factor for developing spider and varicose veins that’s worth mentioning is injury to an area on the leg. Patients often say that a particular patch of spider veins began shortly after they were hit by something e.g. a tennis ball on their thigh. Similarly, varicose veins tend to occur in areas where people have had broken bones and possibly, surgical repair of the fracture. The injury weakens the physical structures in the area surrounding the bone, also affecting the veins.
When to Treat Varicose Veins vs. When to Wait
While the original article focused on causes, patients today often ask when treatment may be recommended instead of simply observing the veins over time. You may want to consider treatment if you are noticing:
- Worsening aching or heaviness in the legs
- Swelling that increases throughout the day
- Nighttime cramping or restlessness
- Itching, irritation, or darkening of the skin
- Tender, inflamed, or sensitive veins
- Visible veins that are enlarging over time
Monitoring may be reasonable if symptoms are mild, stable, and mostly cosmetic. A brief ultrasound assessment can clarify whether your veins are functioning normally or showing signs of progression.
After an ultrasound assessment, most treatments used today are minimally invasive, performed under local anesthetic, designed to close the unhealthy vein so blood can reroute into healthier ones.
There are three categories of treatment:
- Thermal based vein procedures – Endovenous Laser Treatment (EVLT) in our clinic
- Medical adhesive (vein glue) procedures – VenaSeal in our clinic
- Targeted injections for smaller veins – Sclerotherapy or Tumescent Sclerotherapy
When to Seek a Vein Assessment
For a safe and private assessment of your varicose veins, consult Dr. Janna Bentley and the specialized team at Lakeshore Vein & Aesthetics Clinic, located in Kelowna, BC. An updated ultrasound-guided vein consultation can determine whether treatment is recommended now or if monitoring is appropriate.